 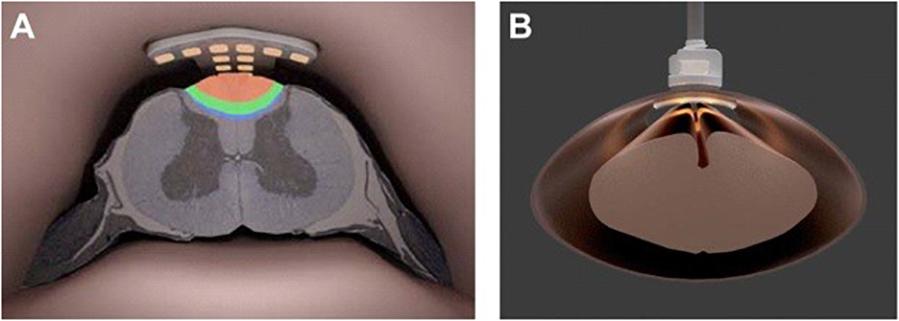
The SCS device consists of an implantable pulse generator connected to 1 or more stimulating leads introduced into the epidural space and positioned at the level where the pain is best inhibited ( Figure 1). The purpose of this review is to summarize the epidemiology and pathogenesis of SCS infections, provide guidance for diagnostic evaluation and management, and discuss strategies for prevention. SCS infection has significant implications for the device recipient, often requiring device removal, preventing patients from receiving adequate pain management and adding to the initial cost and disability. However, mortality associated with SCS implantation is infrequent. Nearly 50% of these complications warrant subsequent surgical revisions. SCS implantation is not without complications, with an overall estimated rate up to 40%. The number of SCS implantations is steadily increasing, and the individual cost associated with these procedures can reach up to $60 000. Indications for SCS use include neuropathic pain, intractable angina, cancer-related pain, complex regional pain syndrome, and painful peripheral arterial disease. SCS consists of implantation of electrodes in the epidural space to alter painful stimuli, originating in the dorsal columns of the spinal cord, to the brain. Patients who fail conservative treatments may be considered for electrical neuromodulation therapy, among which spinal cord stimulation (SCS) is the most commonly utilized technology. Several pharmacological and nonpharmacological therapies are available for management of chronic pain. Spinal cord stimulator, infection, diagnosis, management, prevention Several preventive strategies can be incorporated in surgical practice to reduce the risk of SCS infection. Duration of antimicrobial therapy depends on severity of clinical presentation and presence or absence of associated complications. While superficial surgical site infection following SCS implant may be treated with antibiotic therapy alone, deep infection involving implant warrants device removal to achieve cure. Early recognition of SCS-related infections and associated complications is based on clinical suspicion, laboratory testing, and appropriate diagnostic imaging. However, delay in diagnosis may lead to complications such as meningitis, epidural abscess, and/or vertebral osteomyelitis. Most SCS infections present as generator pocket infection. Infection is one of the most dreaded complications related to SCS implantation and may prevent patients from receiving adequate pain treatment, adding to the initial cost and disability. Spinal cord stimulation (SCS) is the most utilized invasive electrical neuromodulation treatment for the management of refractory chronic pain syndromes. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
